Tooth pain can strike suddenly and become unbearable quickly. One cause of such tooth throbbing is pulpitis, which is a dental condition affecting the inner part of the tooth.
The pulp inside the tooth can become inflamed, leading to sensitivity, severe pain and even infection if treated quickly. Knowing the types of pulpitis, their symptoms, causes, and treatment options can help you identify them early enough to help protect your oral health.
So, have a look at everything you need to know about pulpitis and how dentists can treat it effectively.
Key Takeaways
- Pulpitis is inflammation of the tooth’s inner pulp, most often caused by deep cavities, trauma or a bacterial infection.
- There are two main forms of pulpitis, reversible and irreversible pulpitis, and the difference is whether the pulp can heal.
- Severe or prolonged tooth pain, pain when eating, and sensitivity to hot or cold that lasts too long are all symptoms of irreversible pulpitis.
- Dentists identify pulpitis through clinical examination, temperature sensitivity tests, percussion tests and dental X-rays.
- Reversible pulpitis treatment typically involves removing the cavity and placing a dental filling; in more severe cases, root canal or tooth extraction is required.
- Professional dental clinics, like SmileOn, provide timely treatment for pulpitis that helps avoid worsening of the condition and treat it in time.
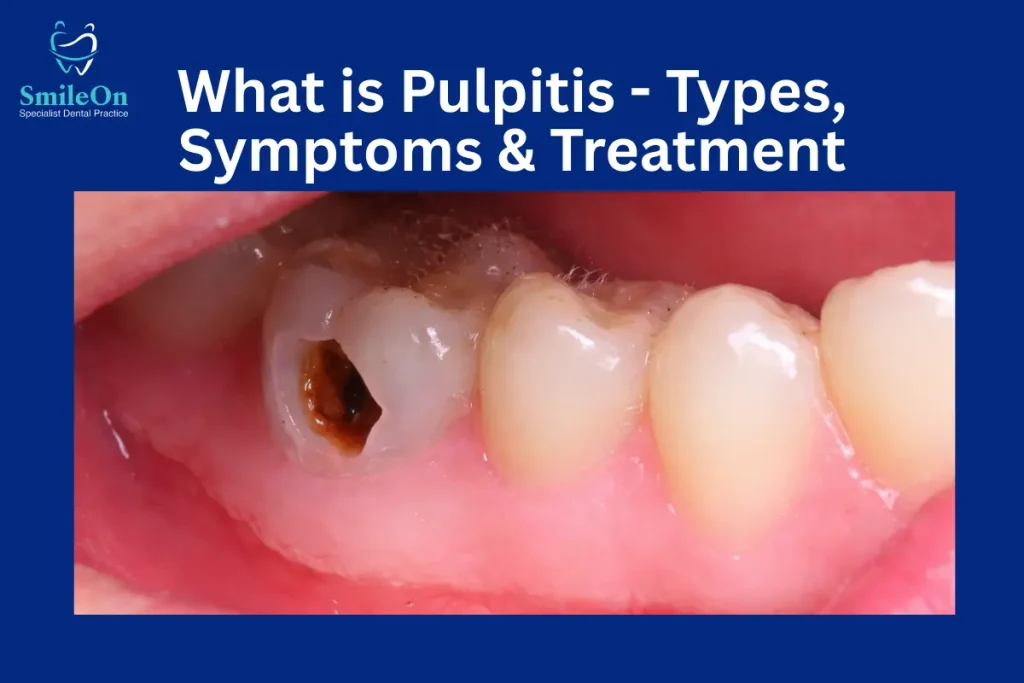
What is Pulpitis?
Pulpitis is the inflammation of the dental pulp, the term for the soft tissue that lies deep in the tooth. The pulp holds nerves, blood vessels and connective tissue that keep the tooth alive and nourished.
When bacteria, trauma or decay all make it to the pulp, the tissue becomes irritated or infected, causing inflammation and pain.
Pulpitis usually occurs from untreated tooth decay or dental damage that allows bacteria to attack the pulp. If caught early, the tooth can often be saved. But, more severe inflammation might need more difficult dental treatment.
What Are the Types of Pulpitis?
There are different classifications for pulpitis depending on the time of inflammation and severity. Knowing the different types of pulpitis allows one to determine the best treatment.
Here is reversible vs irreversible pulpitis:
Reversible Pulpitis
Reversible pulpitis is the least severe type of pulp inflammation. In this phase, the pulp is inflamed but still strong enough to repair itself when the root of the problem is addressed.
Common characteristics include:
- Mild to moderate tooth sensitivity
- Pain triggered by hot, cold or sweet foods
- Discomfort that vanishes fast after removing the stimulus
When treated with good dental hygiene, reverse pulpitis treatment typically includes scraping away the decay near the cavity, followed by a filling to seal and protect the tooth.
Irreversible Pulpitis
Irreversible pulpitis is when the pulp is so inflamed that it cannot heal on its own. At a certain point, the tissue inside the tooth is condemned for good.
Irreversible pulpitis symptoms often include:
- Persistent or severe tooth pain
- Pain occurs without a trigger
- New sensitivity to hot or cold
- Pain that persists long after the stimulus is removed
- Swelling around the affected tooth
And since pulp cannot repair itself at this stage, treatment for pulpitis typically involves a root canal or tooth extraction.
It is further divided into 2 categories, described below:
Difference between acute and chronic pulpitis
Acute Pulpitis
What is an acute pulpitis?
Symptoms usually occur quickly and can include:
- Sharp or throbbing pain
- Sensitivity to temperature changes
- Pain while chewing
- Pain that worsens at night
Chronic Pulpitis
Chronic pulpitis is longer lasting and can be less painful than acute.
Common features include:
- Mild but persistent tooth discomfort
- Occasional sensitivity
- Slow progression of inflammation
In some cases, there may be an initial absence of symptoms allowing condition to worsen.
Common Causes and Risk Factors of Pulpitis
There are a number of dental problems that can cause inflammation in the pulp. Most cases arise when bacteria infiltrate the tooth and contaminate the pulp.
Common causes include:
Tooth Decay
This condition is usually caused by untreated cavities. When decay reaches deep into your tooth, bacteria reach the pulp, where they can cause infection.
Cracked or Fractured Teeth
When this occurs, bacteria are allowed to spread into the inner layers of the tooth, increasing the risk for pulp inflammation.
Repeated Dental Procedures
Repeated dental treatment on the same tooth can irritate the pulp and cause an inflammatory response.
Dental Trauma
Accidents, sports injuries or chewing hard objects can damage the pulp.
Gum Disease
Advanced gum disease can reveal the roots of teeth, which provides an opening for bacteria to move in and infect the pulp.
Poor Oral Hygiene
Poor brushing and flossing contribute to plaque accumulation and dental caries that could also trigger pulpitis.
What are the Signs and Symptoms of Pulpitis?
Identify the symptoms early and prevent the condition from getting worse.
Common pulpitis symptoms include:
- Sensitivity of the teeth to hot or cold foods
- Sharp or throbbing tooth pain
- Pain while chewing or biting
- Swelling in the gums
- Tooth discoloration
- Bad taste in the mouth
- Pain that goes to the jaw, ear or head
Symptoms are often more severe because of the condition being reversible pulpitis versus irreversible pulpitis.
Diagnosis Methods
There are several ways in which dentists diagnose pulpitis and assess how severe the condition is.
Dental Examination:
The dentist will look for cavities, cracks in the tooth, or signs of infection.
Sensitivity Tests:
Specific heat tests with hot or cold materials determine how the pulp responds.
Percussion Test:
The dentist gently taps the tooth to see if there is any pain or inflammation.
Dental X-rays:
Dental X-rays can see inside the tooth and identify infections, decay or pulp damage.
An accurate diagnosis will help dentists determine the best approach to treat pulpitis.
Pulpitis Treatment Options
The type and severity of pulp inflammation determine treatment.
Reversible Pulpitis Treatment
In case of mild pulp damage, the role of dentists is to remove irritation.
Common treatments include:
- Removing tooth decay
- Placing a dental filling
- Replacing damaged fillings
- Shielding the tooth with dental sealants
This pulp usually heals on its own when the cause is removed.
Treatment for Irreversible Pulpitis
For significant damage to the pulp, more comprehensive treatment is necessary.
Root Canal
The most common treatment for pulpitis is an irreversible root canal.
The procedure involves:
- Removing the infected pulp
- Cleaning and disinfecting the root canals
- Filling and sealing the tooth
- Fitting a protective crown on the tooth
In contrast, root canal therapy enables patients to retain their natural tooth and relieve pain or infection.
Tooth Extraction
If it cannot be preserved, the dentist suggests removing the tooth so that the infection can not spread.
Once out, the lost tooth may be replaced with:
How to Manage Pain? Effective Tips
Dentists can also suggest temporary pain relief methods, including:
- Over-the-counter pain medications
- Antibiotics for infection
- Avoiding foods that are very hot or cold
- Maintaining good oral hygiene
But improving the pain does not make pulpitis go away. However, you still need professional dental treatment.
How to Prevent Pulpitis?
Pulpitis prevention is largely based on oral health care and the early elimination of dental pathology.
Helpful prevention tips include:
- Twice a day, brush teeth thoroughly for two minutes using fluoride toothpaste.
- Floss daily to help prevent plaque buildup
- Have regular check-ups with the dentist
- Treat cavities promptly
- Avoid chewing hard objects
- Wear a mouth guard during sports
However, regular trips to the dentist can catch issues before they reach the pulp.
Conclusion
All in all, tooth pain should never be ignored, particularly when the underlying issue may be pulpitis, an inflammation of the sensitive inner pulp of the tooth.
Knowing the different types of pulpitis, early recognition of symptoms and professional dental care can help to prevent serious complications. While reversible pulpitis is often treated with minor interventions, irreversible pulpitis may require more advanced treatment including a root canal.
However, if you are feeling persistent pain or sensitivity in your teeth, experienced dentists at SmileOn can help diagnose and treat the issue early by providing the right treatment to restore your oral health and comfort.
FAQs
Is pulpitis the same as an abscess?
No, pulpitis is when the dental pulp becomes inflamed; a dental abscess is an accumulation of pus in the surrounding tissues caused by bacterial infection. If pulpitis is left untreated, it may sometimes cause an abscess.
Does pulpitis go away by itself?
Mild reversible pulpitis may resolve on its own once the cause is treated, but it almost never goes away without some sort of dental care. Irreversible pulpitis does not heal naturally or spontaneously and thus requires professional care.
What is the best treatment for pulpitis?
Its severity determines the best treatment. The treatment of reversible pulpitis typically involves the removal of decay and a filling, whereas irreversible pulpitis often requires a root canal, or in some cases, tooth extraction.